An elderly female patient was admitted to a hospital for surgery following a hip fracture at home. On admission, the patient’s skin was intact and she had no pressure ulcers (also called pressure sores, bed sores, or decubitus ulcers). The patient was discharged from the hospital approximately one week later. At the time of discharge, the patient was documented to have three small open areas on her right buttock near the lower back. The patient was discharged from the hospital to a nursing home, which documented the patient to have open “excoriation” on her lower back. The nursing home otherwise assessed the patient as a “low risk for pressure ulcer development.”
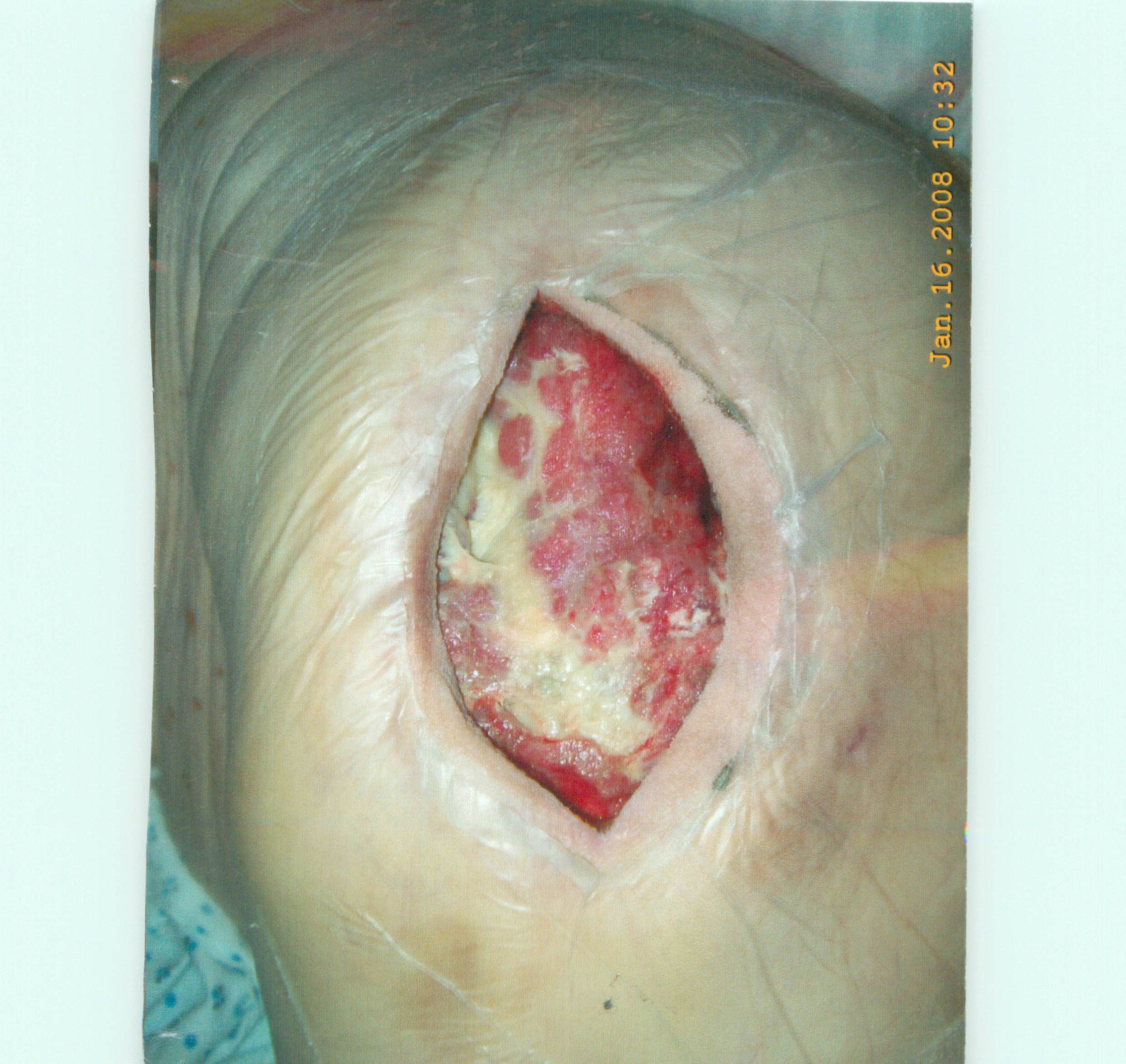
The patient was later transferred from the nursing home back to the hospital because the pressure ulcer had become infected. The patient had also developed a new pressure ulcer on her left hip. At the hospital, infection of the pressure ulcer was noted to have extended into the left hip hardware. The patient required multiple surgical debridements for the sacral and left hip pressure ulcers. She also experienced what was described in her medical records as “unbearable” pain in her buttock as a result of the sacral ulcer. The patient also required a wound vac and antibiotics. The patient was discharged from the hospital to a new nursing home, where her antibiotic therapy and wound care continued, she received therapy services, and where she remains today.
We claimed that the hospital and nursing home failed to provide proper pressure ulcer prevention and care. Specifically, the hospital and nursing home failed to turn and reposition the patient as often as was necessary, often left the patient positioned on existing pressure ulcers, and failed to apply and use properly the wound vac, all of which caused the pressure ulcers to develop and deteriorate.
The hospital and nursing home settled well before trial for a combined settlement in the mid-to-high six figures.
Robert W. Carter, Jr. is a Virginia attorney whose law practice is dedicated to protecting the rights of the victims of nursing home and assisted living neglect and abuse in Richmond, Roanoke, Norfolk, Lynchburg, Danville, Charlottesville, and across Virginia.

